|
|
|
Indian Pediatr 2015;52:
987-988 |
 |
Klippel-Trenaunay-Weber Syndrome with Kasabach-Merritt
Coagulopathy and Hydronephrosis
|
|
Lata Bhat, Supriya Bisht and Kavita Khanijo
From Department of Neonatology, Fortis Hospital,
Noida, Uttar Pradesh, India.
Correspondence to: Dr Supriya Bisht,
Department of Neonatology, Fortis Hospital, B-22, Sector 62,
Noida, Uttar Pradesh, India.
Email:
[email protected]
Received: March 04, 2015;
Initial review: June 05, 2015;
Accepted: August 28, 2015 .
|
|
Background: Klippel-Trenaunay-Weber
Syndrome is a rare syndrome, consisting of vascular malformation of
blood and lymph vessels. Case characteristics: A newborn female
with respiratory distress from birth, and having vascular malformation
involving left thigh. Observation: The neonate also had
hydronephrosis and developed complication of Kasabach Merritt syndrome.
Message: Urogenital abnormalities can be present in Klippel-Trenaunay-Weber
syndrome but hydronephrosis is rare. Mortality is high with development
of Kasabach Merritt syndrome.
Keywords: Bleeding neonate, Coagulopathy,
Neonate, Vascular malformation.
|
|
Klippel-Trenaunay-Weber syndrome (KTWS) consists
of combined vascular malformation of the capillary, venous and lymphatic
types[1]. Varicosities of unusual distribution is observed during
infancy or childhood, along with limb enlargement [2]. Hypertrophy of
the soft or hard tissues results in asymmetry of the involved extremity
[3]. The clinical presentation can be extremely variable. Although
urogenital abnormalities can be present, hydronephrosis is rare in KTWS
[4]. Kasabach-Merritt syndrome, a consumptive coagulopathy, can
complicate around 45% of cases of KTWS. High output cardiac failure in
KTWS is usually secondary to anemia and large arterio-venous
malformation [5]. We present a case of KTWS with hydronephrosis, who
developed Kasabach-Merritt syndrome.
Case Report
A newborn female was referred to our hospital at six
hours of life with complaints of respiratory difficulty since birth, and
enlarged left thigh with vascular malformation. She was born by
caesarian section at 36 weeks gestation, and cried immediately after
birth. Her weight was 3.5 kg. Mother had infrequent antenatal check-up
and an unremarkable medical history.
At admission, she had tachycardia, tachypnea,
grunting, prolonged capillary refill time, hypoxia (SpO 2
85% on oxygen by prongs) and feeble pulses. Systemic examination
revealed bilateral crepitations, grade III systolic murmur at upper
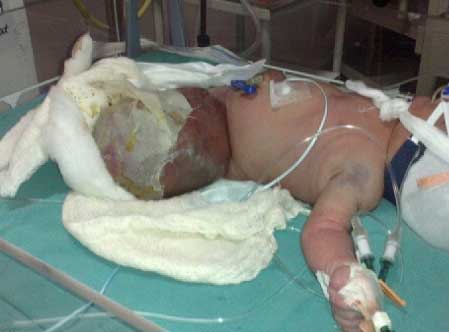
right sternal border, and a palpable liver (2.5 cm). There was a large
vascular malformation on the left thigh with splitting of overlying skin
(Fig. 1). There was no other anomaly or dysmorphism.
Investigations were suggestive of anemia (hemoglobin 7.5 g/dL) and
severe thrombocytopenia (platelet count: 8×109/L).
Total leucocyte count (13.3 ×109/L),
serum electrolytes and serum calcium were normal; C-reactive protein was
negative.
 |
|
Fig.1 Large arterio-venous
malformation affecting left thigh.
|
| |
 |
|
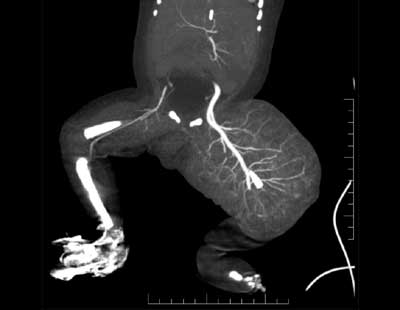
Fig. 2 Coronal image of CT angiography
showing large soft tissue swelling of left thigh and multiple
arterial feeders along with dilated femoral artery.
|
She received intravenous antibiotics, packed red
cells, platelet concentrates and fresh frozen plasma. Intravenous
furosemide was administered in view of congestive heart failure. By 12
hours of life, infant’s condition remained critical, and she required
mechanical ventilation. X-ray chest showed cardiomegaly (CT ratio
0.7), and liver was palpable (3 cm below costal margin). Congestive
cardiac failure further worsened, requiring digitalization and inotrope
support to maintain perfusion. Echocardio-graphy revealed dilated right
atrium, right ventricle and major pulmonary artery, mild to moderate TR,
small ASD, and PDA. Doppler ultrasound of the enlarged left lower limb
showed large arterio-venous malformation from left inguinal region
including labia, extending upto foot. Computed tomography (CT)
angiography of the affected left thigh revealed tufts of vessels in
subcutaneous planes arising from superficial femoral artery, with
enhancing soft tissue component and large draining veins sugges-tive of
large arterio-venous malformation (Fig. 2). Urinary
bladder was also grossly distended with bilateral hydronephrosis.
Interventional radiologist suggested angio-embolization of the affected
arterio-venous malformations, but the parents refused the procedure.
Steroids were not administered because of fulminant sepsis. Child’s
condition worsened and coagulation profile deteriorated further. She
developed pulmonary hemorrhage and died on day four of life due to
severe bleeding manifestations, overwhelming sepsis and cardiac failure.
Discussion
Kasabach-Merritt syndrome, a potentially
life-threatening coagulopathy characterized by enlarging hemangioma with
severe thrombocytopenia [6], can complicate KTWS. Analysis of prenatal
presentations and perinatal outcomes of KTWS suggested that the
involvement of fetal thigh is rare [7]. Bilateral hydronephrosis is very
rarely reported with KTWS [4]. Although urine output and renal function
tests were normal, further workup of renal system involvement could not
be done. Mortality rate in the neonatal period is high with
complications of Kasabach-Merritt syndrome observed in about one-third
of cases [7]. The causes of
neonatal mortality in KTWS includes Kasabach-Merritt syndrome, cardiac
failure, sepsis, and prematurity [7,8]. Treatment options include
steroids, compression, pulsed-dye laser treatment, surgical reduction or
embolization. Surgical therapy is often precluded by the risk of severe
hemorrhage and high mortality in extensive lesions [7].
Contributors: LB: Patient management. SB:
manuscript writing.; KK: investigation support and the care of the
patient.
Funding: None; Competing interest: None
stated.
References
1. Weber FP. Angioma formation in connection with
hypertrophy of limbs and hemihypertrophy. Br J Dermatol. 1907;19:231.
2. Cohen MM. Klippel Trenaunay syndrome. Am J Med
Genet. 2000;93:171-5.
3. Huang WJ, Creath CJ. Klippel-Trenaunay syndrome:
literature review and case report. Pediatr Dent.1994;16:231-5.
4. Yildizdas D, Antmen B, Bayram I, Yapicioglu H.
Klippel-trenaunay-Weber syndrome with hydronephrosis and vesicoureteral
reflux: An unusual association. Turk J Pediatr. 2002;44:180-2.
5. Samuel M, Spitz L. Klippel-Trenaunay syndrome:
Clinical features, complications and management in children. Br J Surg.
1995;82:757-61.
6. Kasabach HH, Merritt KK. Capillary hemangioma with
extensive purpura: Report of a case. Am J Dis Child. 1940;59:1063-70.
7. Peng HH, Wang TH , Chao AS , Chang YL , Shieh SC,
Chang SD. Klippel-Trenaunay-Weber syndrome involving fetal thigh:
Prenatal presentations and outcomes. Prenat Diagn. 2006;26:825-30.
8. Zoppi MA, Ibba RM, Floris M, Putzolu M, Crisponi
G, Monni G. Prenatal sonographic diagnosis of Klippel-Trénaunay-Weber
syndrome with cardiac failure. J Clin Ultrasound. 2001;29:422-6.
|
|
|
 |
|

