|
|
|
Indian Pediatr 2014;51: 401 -402 |
 |
Multidrug-resistant Tubercular Liver Abscess in
β-thalassemia
|
|
Amit Agrawal, Jyotsna Shrivastava and Akhil Singh
From Department of Pediatrics, Gandhi Medical
College and Kamla Nehru Hospital, Bhopal, MP, India.
Correspondence to: Dr Amit Agrawal, 28, Ravidas
Nagar, Near Nizamuddin Colony, Indrapuri,
Bhopal, MP 462 023, India.
Email:
agrawaldramit@yahoo.co.in
Received: December 02,2013;
Initial review: January 02, 2014;
Accepted: March 07, 2014.
|
|
Background: Liver abscesses in thalassemics are predominantly
pyogenic. Case characteristics: 12-year-old thalassemic boy with
abdominal pain and high grade fever for 15 days. Observation: CT
abdomen revealed multiple liver abscesses. Pus culture and sensitivity
showed multidrug-resistant mycobacteria. Patient was started on second
line anti-tubercular drugs. Outcome: He responded well with
symptomatic improvement and is doing well after 6 months of follow-up.
Message: Liver abscess in patients with thalassemia rarely can be
tubercular.
Keywords: Liver abscess, Mycobacterium
tuberculosis, Thalassemia major.
|
|
P
rimary tubercular liver abscess (TLA) is rare,
even in countries with high prevalence of tuberculosis (TB) [1-4].
Thalassemics have co-existent immunodeficiency that makes them more
susceptible to infection-related morbidity and mortality [5-6]. Liver
abscesses in patients with thalassemia are predominantly pyogenic;
tubercular abscesses are very rare. We report a case of tubercular liver
abscess in a child with thalassemia.
Case Report
A 12-year-old boy presented with dull aching pain in
right upper abdomen and lower chest associated with intermittent
high-grade fever, weakness and vomiting for 15 days. He was suffering
from b-thalassemia
major receiving frequent but inadequate blood transfusions for 11 years,
and iron chelation therapy (deferasirox) for 2 years. There was no past
history of tuberculosis or contact with a patient of tuberculosis. On
physical examination, patient was sick, febrile (102.60F)
and pale; pulse rate was 88/min, blood pressure was 104/66 mmHg and
respiratory rate was 22/min. Tenderness was present in right
hypochondrium; liver and spleen were markedly enlarged. There was no
ascites or other palpable mass. Respiratory and cardiovascular
examination were normal.
On investigation, hemoglobin was 7.7 g/dL, total
leucocyte count was 16000/mm 3
and peripheral smear showed microcytic hypochromic anaemia. Chest X-ray
was normal, Mantoux test was negative and three early morning sputum
samples were negative for acid-fast-bacilli (AFB). Serum ferritin was
markedly elevated (2450 mg/dL). Rest of the investigations (including
widal test, malarial antigen, urine routine and culture, blood culture
HbsAg, Anti HCV, and HIV-ELISA) were within normal limits. Abdominal
ultrasound showed heterogeneous, ill-defined, hypo-echoic lesions
reaching upto liver surface in right lobe of the liver suggestive of
multiple abscesses. No perihepatic or pleural effusion was seen. A
clinical diagnosis of pyogenic liver abscess was made and patient was
put on intravenous antibiotics but his fever and abdominal pain
persisted even after two weeks of therapy. Repeat ultrasound abdomen
showed similar findings. Computed tomography (CT) of abdomen revealed
multiple hypodense lesions with peri-lesional enhancement in right lobe
of liver suggestive of multiple abscesses (Fig. 1). Pus
was aspirated under CT-guidance and sent for examination and culture.
Zeil-Neilsen staining and culture demonstrated Acid fast bacilli (AFB)
in aspirated pus; there were no amebic trophozoites or fungal elements.
Anti-tubercular therapy (ATT) with isoniazid, rifampicin, pyrazinamide,
and ethambutol was started along with supportive therapy. Fever and
abdominal pain gradually subsided with improvement in his appetite and
general condition. However, after 4 month of regular ATT, patient
presented again with abdominal pain and intermittent fever. He had a pus
discharging sinus in the right hypochondrium. Repeat ultrasound and CT
abdomen revealed multiple liver abscesses. Pus culture and sensitivity
revealed multidrug-resistent tuberculosis (MDR-TB) as organisms were
resistant to both isoniazid and rifampicin. Patient was put on kanamycin,
ofloxacin, para-amino-salicyalate, etambutol and pyrizinamide, to which
he responded well with symptomatic improvement and cessation of
discharge. At 6 months of follow-up, he was doing well.
 |
|
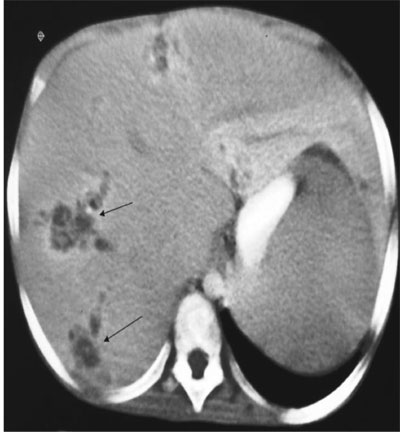
Fig. 1 CT abdomen showing
multiple hypodense lesions (black arrows) with peri-lesional
enhancement in right lobe of liver suggestive of multiple
abscesses.
|
Discussion
Ruptured tubercular liver abcess presenting as
parietal wall swelling is extremely rare with only few reported cases
[1-4], that too in adults. Primary liver involvement as tubercular liver
abcess is also very rare. Route of infection is usually hematogenous;
respiratory and gastrointestinal tracts are primary sources of infection
[7,8]. Clinical manifestations of tubercular liver abcess are
nonspecific and include anorexia, fever, and vague/localized right upper
quadrant pain. Hepatomegaly is common on presentation but jaundice due
to extra or intrahepatic obstruction is rare [7,8].
Co-existent immunodeficiency in thalassemic children
– both humoral and cell mediated – make them prone to infections. Iron
excess deranges the immune system to favor the growth
of infectious agents. Other factors include splenectomy resulting in
increased susceptibility to encapsulated bacterial infections,
transfusion-related allo-antigenic stimulation, trans-mission of
immunosuppressive viruses, iron chelation therapy predisposing to
yersinia infections, and zinc deficiency [5-6]. Wang, et al. [9]
reported 1.6 episodes of severe bacterial infections/100 patient-years
in transfusion dependent thalassemic patients with liver being the most
common focus, and likely organisms were gram negative bacteria.
Tuberculosis in thalassemics can be explained by deficient cell mediated
immunity and altered immunological profile. Our case was not
splenectomized but was inadequately transfused and iron overloaded with
irregular chelation therapy making him prone to infections.
Clinicians should be aware of unusual co-morbidities
in thalassemics, and surveillance for infections is crucial to improve
the survival and quality of life. Tubercular liver abscess, although
very rare, should be considered in differential diagnosis of hepatic
mass lesions, especially multi-loculated abscess in immuno-compromised
patients.
Contributors: AA: Literature review,
manuscript review, manuscript editing, and patient management; JS:
Manuscript editing, patient management, and revising the article
critically for important intellectual content; AS: Acquisition and
interpretation of data, literature search and review, and drafting the
article. JS will act as guarantor. All authors approved the final
manuscript.
Funding: None; Competing interests:
None stated.
References
1. Abe K, Aizawa T, Maebayashi T, Nakayama H,
Sugitani M Sakaguchi M, et al. Isolated tuberculous liver
abscess invading the abdominal wall: report of a case. Surgery Today.
2011;41:741-4.
2. Desai N, Patil S, Thakur BS, Das HS, Manjunath SM,
Sawant P. Abdominal wall abscess secondary to subcapsular tubercular
liver abscess. Indian J Gastroenterol. 2003;22:190-1.
3. Gupta G, Nijhawan S, Katiyar P, Mathur A. Primary
tubercular liver abscess rupture leading to parietal wall abscess: A
rare disease with a rare complication. J Postgrad Med. 2011;57:350-2.
4. Mohanty D, Jain BK, Gupta A, Agrawal V. Chest wall
abscess: An atypical presentation of isolated tuberculous liver abscess.
Acta Biomed. 2009;80:77-9.
5. Olivieri NF, Weatherall DJ. Thalassemias. In:
Arceci RJ, Hann IM, Smith OP, eds. Pediatric Hematology. 3rd ed.
Oxford, UK: Blackwell Publishing Ltd; 2006. p. 281- 304.
6. Farmakis D, Giakoumis A, Polymeropoulos E,
Aessopos A. Pathogenetic aspects of immune deficiency associated with
beta-thalassemia. Med Sci Monit. 2003;9:19-22.
7. Sherlock S, Dooley J. Tuberculosis of liver. In:
Sherlock (Ed), Diseases of the Liver and Biliary System, 11th
edition, Oxford: Blackwell Science, 2002. p. 501.
8. Chaudhary A, Wakhlu A. Isolated tubercular liver
abscess in pediatric age group. Int J Trop Med. 2005;2:2.
9. Wang SC, Lin KH, Chem JP, Lu MY, Jou ST, Lin DT,
et al. Severe bacterial infection in transfusion-dependent
patients with thalassemia major. Clin Infect Dis. 2003;37:984-8.
|
|
|
 |
|

