|
|
|
Indian Pediatr 2015;52:
523-525 |
 |
Acute Kidney Injury Following Plastic
Bronchitis Associated with Influenza B Virus in a Child with
Nephrotic Syndrome
|
|
Shuichiro Fujinaga and Taichi Hara
From Division of Nephrology, Saitama Children’s
Medical Center, Japan.
Correspondence to: Dr Shuichiro Fujinaga,
Division of Nephrology, Saitama Children’s Medical Center,
2100 Magome, Iwatsuki-ku, Saitama-city Saitama 339 8551, Japan.
Email: [email protected]
Received: December 20, 2014;
Initial review: January 27, 2015;
Accepted: April 08, 2015.
|
|
Background: Plastic bronchitis is a rare but life-threatening
disorder and is usually associated with congenital heart disease or
pulmonary disease. Case characteristics: A 5-year-old boy with
minimal change nephrotic syndrome who developed a relapse along with
cough, fever and dyspnea. Observation: Chest X-ray showed
atelectasis of right upper lobe of lung, and nasal swab was positive for
influenza B virus. His respiratory condition worsened, and required
ventilation; bronchoscopy revealed bronchial casts. This was followed by
acute kidney injury which was successfully managed with hemodialysis.
Message: Children with nephrotic syndrome on immunosuppressive
agents can develop plastic bronchitis and acute kidney injury, following
influenza virus infection.
Keywords: Acute kidney injury, Influenza B
virus, Minimal change nephrotic syndrome.
|
|
A
cute kidney injury (AKI), requiring dialysis, is
an uncommon complication of childhood idiopathic nephrotic syndrome.
Plastic bronchitis is an extremely rare and life-threatening disorder
characterized by formation of large gelatinous branching airway casts,
and is usually associated with congenital heart disease and pulmonary
disease [1]. Plastic bronchitis has also been reported with pandemic
2009 influenza A virus infection [2-4]. We report a child with initial
steroid-resistant minimal change nephrotic syndrome who developed
relapse and AKI requiring dialysis, following plastic bronchitis
associated with seasonal influenza B virus infection.
Case Report
A 5-year-old boy with refractory nephrotic syndrome
was admitted to our hospital because of the 5th relapse of nephrotic
syndrome and dyspnea. On admission, his regular medication consisted of
mizoribine and alternate-day prednisolone (10 mg/day). The patient had
not been vaccinated against influenza. At the age of 2 years, the
patient was diagnosed with initial steroid-resistant NS, and thus we
performed first renal biopsy with histology showing minimal change
disease (MCD). Thereafter, complete remission of NS was achieved with
three courses of intravenous methylprednisolone pulses (20 mg/kg/day,
total 9pulses) and cyclosporine A (6-7 mg/kg/day). However, after
reduction in dose of steroids, frequent relapses of nephrotic syndrome
occurred and single infusion of rituximab (375 mg/m 2)
was given, resulting in withdrawal of steroids. The B-cell depletion
period (defined by the time from rituximab treatment until the detection
of CD19+ cells count >1% of total lymphocytes) was 5 months and the B
cell count had recovered at the time of influenza B virus infection. A
protocol renal biopsy 2 years after cyclosporine A treatment showed MCD
and cyclosporine A-associated arteriolopathy, which prompted us to
switch from cyclosporine A to mizoribine.
The patient had no history of congenital heart
disease or chronic pulmonary disease. The day before admission, he had
cough, fever, and wheeze. On arrival in our emergency room, he had
fever, tachypnea and reduced breath sounds in the right hemithorax. A
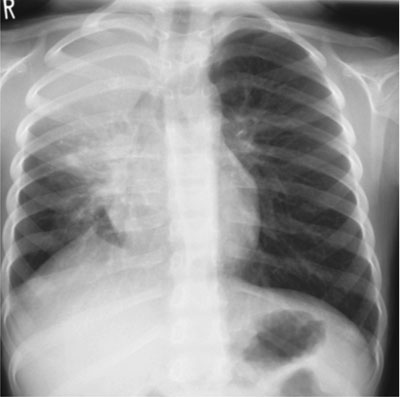
chest X-ray showed atelectasis of the right upper lung (Fig.
1). Laboratory investigations were as follows: white blood cell
count, 11,200/mm 3 (neutrophils,
81.1%; lymphocytes, 10.8%, monocytes, 7.0%; eosinophils, 1.1%);
hemoglobin, 12.6 g/dL; platelet count, 329,000/mm3;
and C-reactive protein level, 5.16 mg/dL. Urinalysis showed 3+ protein
by dipstick. The rapid nasal swab influenza antigen test was positive
for influenza B virus.
 |
|
Fig. 1 Chest radiograph on admission,
showing atelectasis of the upper right lung with a mediastinal
shift to the right.
|
Based on these findings, a presumptive diagnosis of
relapse of nephrotic syndrome following pneumonia associated with both
influenza B virus was made. The patient was treated with intravenous
peramivir, antibiotics, steroids, and continuous inhalation of
isoproterenol with supplemental oxygen. However, he responded poorly to
treatment and his general condition deteriorated. On day 5 of
hospitalization, generalized edema developed and blood examinations
showed hypoproteinemia (total protein, 4.1 g/dL; albumin, 1.2 g/dL) and
hemoconcentration (hemoglobin, 15.3 g/dL; hematocrit, 44.9%), whereas
his renal function was normal at that time (serum creatinine
concentration 0.24 mg/dL). The patient received infusion of 25% albumin
because of decreased radiographic cardiothoracic ratio (38%) and poor
peripheral perfusion (capillary refilling time >2 seconds) suggested
presence of hypovolemia. Although respiratory support by mechanical
ventilation was initiated, breath sounds in the right lung were not
audible and chest X-ray showed mediastinal emphysema and
subcutaneous pneumatosis, in addition to atelectasis. Therefore, a
flexible bronchoscopy at the bedside was performed and bronchial casts
were extracted from the right bronchus, leading to the diagnosis of
plastic bronchitis. A second bronchial aspiration was performed the
following day with further removal of the mucus plugging. After
bronchial aspiration, oxygen saturation increased and chest radiography
revealed marked improvement. On day 7 of hospitalization, the patient
had raised blood urea nitrogen (57 mg/dL) and serum creatinine
concentration (0.67 mg/dL). Oliguria (<0.5 mL/kg/h) continued for more
than 12 hours despite the presence of hypervolemia (hypertension and
increased radiographic cardiothoracic ratio 55%) after infusion of
albumin, which prompted us to initiate continuous venovenous
hemodialysis at bedsides using pediatric devices (TR-55X, Toray Co.,
Tokyo, Japan) and hemofilter (EXCELFRO AEF-03, Asahi medical Co., Tokyo,
Japan). On day 11 of hospitalization, dialysis was discontinued because
urine output increased, and extubation was performed the following day.
Complete remission of NS was achieved with prednisolone (2 mg/kg/day),
and he was discharged three weeks after admission.
Discussion
Plastic bronchitis is an unusual cause of acute
respiratory failure in children that can mimic status asthmaticus. In
our patient, the ineffectiveness of inhaled
b-agonists and
steroids made us suspect this disorder. Recent studies indicate that a
novel influenza A (H1N1), in which mucociliary clearance is more
severely disturbed than in seasonal influenza virus may cause plastic
bronchitis, irrespective of presence or absence of underling
cardiopulmonary disease [2-4]. However, in our patient, seasonal
influenza B virus induced severe plastic bronchitis. Ding, et al.
[5], recently reported influenza B virus in three of nine Chinese
children with plastic bronchitis; two of their patients developed renal
failure. The reason why a simple seasonal influenza virus infection can
cause plastic bronchitis is unclear. Plastic bronchitis has been
reported in patients with Fontan physiology that is often accompanied by
protein-losing enteropathy [6,7]. Hypoalbuminemia seen in our patient
might have altered lymphatic flow leading to development of airway
casts. Bronchial casts could be inflammatory (which occur in patients
with cyanotic heart disease) or acellular (which occur during or
following pneumonia and asthma) [8]. Histologic examination of bronchial
casts was not performed in our patient. Intravascular volume depletion
secondary to low serum albumin concentration and aggressive diuretic
therapy during severe relapse of nephrotic syndrome may promote the
formation of sticky bronchial casts. Narrowing of bronchi with mucosal
edema in association with hypoalbuminemia might have led to the
development of plastic bronchitis.
We speculate that influenza B infection under the
aggressive immunosuppression (mizoribine and prednisolone) was
associated with severe relapse of nephrotic syndrome leading to
reversible idiopathic AKI in our case. However, exact pathogenesis of
AKI remains unclear because renal biopsy at that time was not performed
in our patient. Influenza virus has been associated with exacerbations
and relapse of nephrotic syndrome, especially in unstable patients [10].
Our case demonstrates that the risk of plastic bronchitis and AKI should
be kept in mind when children with nephrotic syndrome on
immunosuppressive agents suffer from seasonal influenza virus infection.
Contributors: All authors have contributed to
patient management and manuscript writing.
Funding: None; Competing interests: None
stated.
References
1. Brogan TV, Finn LS, Pyskaty DJ, Redding GJ, Ricker
D, Inglis A, et al. Plastic bronchitis in children: A case series
and review of the medical literature. Pediatr Pulmonol. 2002;34:482-7.
2. Deng J, Zheng Y, Li C, Ma Z, Wang H, Rubin BK.
Plastic bronchitis in three children associated with 2009 influenza A
(H1N1) virus infection. Chest. 2010;138: 1486-8.
3. Hasegawa M, Inamo Y, Fuchigami T, Hashimoto K,
Morozumi M, Ubukata K, et al. Bronchial casts and pandemic (H1N1)
2009 virus infection. Emerg Infect Dis. 2010;16:344-6.
4. Terano C, Miura M, Fukuzawa R, Saito Y, Arai H,
Sasaki M, et al. Three children with plastic bronchitis
associated with 2009 H1N1 influenza virus infection. Pediatr Infect Dis
J. 2011;30:80-2.
5. Ding XF, Zhong LL, Zhang B, Lin L, Huang H, Liang
M. Clinical features and pathogens of plastic bronchitis in children: an
analysis of 9 cases. Zhongguo Dang Dai Er Ke Za Zhi. 2014;16:729-33.
6. Stiller B, Riedel F, Paul K, van Landeghem FKH.
Plastic bronchitis in children with Fontan palliation: Analogue to
protein losing enteropathy? Pediatr Cardiol. 2002;23:90-4.
7. Rychik J, Goldberg D, Rand E, Semeao E, Russo P,
Dori Y, et al. End-organ consequences of Fontan operation: Liver
fibrosis, protein-losing enteropathy and plastic bronchitis. Cardiol
Young. 2013;23:831-40.
8. Seear M, Hui H, Magee F, Bohn D, Cutz E. Bronchial
casts in children: A proposed classification based on nine cases and a
review of the literature. Am J Respir Crit Care Med. 1997;155:364-70.
9. Agarwal N, Phadke KD, Garg I, Alexander P. Acute
renal failure in children with idiopathic nephrotic syndrome. Pediatr
Nephrol. 2003;18:1289-92.
10. MacDonald NE, Wolfish N, McLaine P, Phipps P,
Rossier E. Role of respiratory viruses in exacerbations of primary
nephrotic syndrome. J Pediatr. 1986;108: 378-82.
|
|
|
 |
|

