|
A 1½-year-old boy who is followed up in our Nutrition and Growth
Clinic was diagnosed to have co-existent osteopetrosis and rickets. At
the time of diagnosis, he was seven months old and had anthropometric
parameters below the 3rd centile of the NCHS reference standards
except head circumference, which was between the 25th and the 50th
centile. Clinical examination revealed pallor, hepato-splenomegaly,
early optic atrophy and features of rickets like caput quadratum, wide
open anterior and posterior, fontanels, Harrison’s sulcus, rachitic
rosaries and widening of wrists and ankles. Laboratory data showed
hemoglobin 7.5 g/dL, total leukocyte count of 11,200/cumm, polymorphs
52%, lymphocytes 30% and eosinophils 18%, platelet count 1 lakh/cumm
and leuko- erythroblastic blood picture with mild thrombocytopenia. He
had normal thyroid function and normal karyotyping. The serum calcium
(7.2 mg/dL) and phosphorus (1.4 mg/dL) levels were low and alkaline
phosphatase (2005 IU/L) was markedly raised. Serum sodium, potassium,
bicarbonate and urine pH were normal and associated renal tubular
acidosis was excluded. Urine was negative for mucopolysaccharides and
aminoaciduria. The liver and renal function tests were within the
normal range. Skeletal survey revealed features of osteopetrosis,
rickets and pathological fractures with ‘bone in bone’ appearance,
increase in medullary density, defective metaphyseal remodeling with
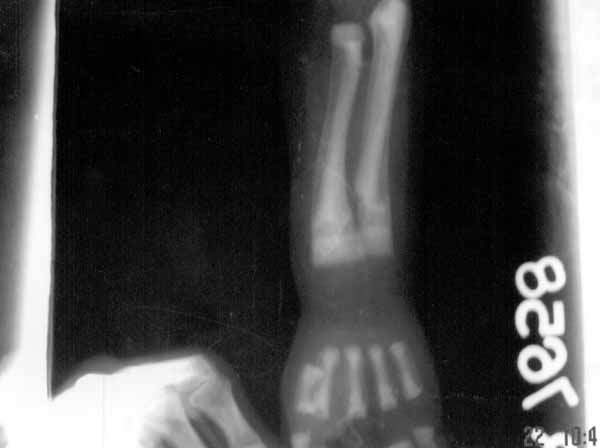
fraying and early cupping and widening of ‘physis’, the growth plate (Fig.1).
US$ showed hepatosplenomegaly and CT scan head showed osteosclerosis
and diffuse brain atrophy.
 |
|
Fig. 1. X-ray of left forearm and hand
showing osteosclerosis, ‘bone in bone’ appearance of shaft,
fracture both bones, fraying and early cupping of metaphysis and
widening of ‘physis’, the growth plate and absence of carpal
bones. |
Osteopetrorickets is a rare association of
osteopetrosis with rickets(1,2). In osteopetrosis, there is excess
calcium reserve and hypophosphatemia(3), but when it is complicated by
rickets there is an insufficient Ca:P product to mineralize the
growing bone. In coexistent osteopetrosis and rickets, 99% of the
calcium is shut off in the bone and is not available as a source of
these minerals and the calcium phosphorus product will become <40,
thus insufficient for mineralisation. In such cases, there is chance
for hypocalcemic tetany(3). This association is considered a paradox
in the midst of plenty(4). Low calcium and high phosphate diet
prescribed in osteopetrosis may further decrease the availability of
calcium and in rickets liberal calcium is required. Low dose steroid
therapy, which is found effective in treating and preventing the
hematological problems in osteopetrosis may blunt the intestinal
response to maximal vitamin D stimulation as well(4). The general view
is to treat rickets in this co-morbid situation as it will improve
well being, decrease irritability and decrease infections. This may
also help in preparing the patient for future bone marrow
transplantation which is the ultimate therapy in osteopetrosis.
Initially, before complete work up, the child was
on low calcium, high phosphorus diet and phosphate supplement in the
form of Joulie solution. After the confirmation of associated rickets,
he was given 2 loading doses of vitamin D3, 6 lakhs units at 3 weeks
interval, but there was no line of calcification. Later, he was put on
liberal calcium and phosphorus diet with extra calcium carbonate
supplements up to 200 mg/kg per day, Joulie solution 4 g/day in 5
doses and 2 mcg/day of 1,25 dihydroxy cholecalciferol. He was also on
1 mg/kg oral prednisolone on an alternate day basis. After three
months, serum calcium became 9.4 mg/dL and phosphorus 3.3 mg/dL and
serum alkaline phosphatase 677 IU/L and X-ray showed features
of healing. The general well being of the child has improved. Growth
is continuing in the 3rd centile and he is able to stand with support
at 18 months of age. Tooth eruption was delayed up to 18 months.
K. E. Elizabeth,
Gibby Koshy,
Department of Pediatrics,
SAT Hospital,
Government Medical College,
Trivandrum 695 011, Kerala,
India.
E-mail: [email protected]
1. Datta V, Prajapati NC, Kamble M, Pathak S.
Osteopetrorickets. Indian Pediatr 2000, 37: 98-99.
2. Oliveira G, Boechat MI, Amaral SM, Young L W.
Osteopetrosis and rickets: An intriguing association. Am J Dis Child
1986, 140: 377-378.
3. McCary LC, Smith CM, DeLuca HF.
Hypophosphatemia and the development of rickets in osteopetrotic
mice. J Bone Mineral Dis 1997, 12: 1944-1951.
4. Kapla FS, August CS, Fallon MD, Cannon F, Haddad JG.
Osteopetrorickets, the paradox of plenty. Pathophysiology and
treatment. Clin Orthop 1993, 294: 64-68.
|
