|
|
|
Indian Pediatr 2009;46: 178-180 |
 |
Prolonged Hungry Bone Syndrome in a
10-year-old Child with Parathyroid Adenoma |
|
Enver Simsek, Yasemin Arikan, Yildiz Dallar, and Mehmet
Ali Akkus*
From the Departments of Pediatric Endocrinology and
*Surgery, Ankara Research and Training Hospital,
Ulucanlar, Ankara, Turkey.
Correspondence to: Associate Prof Enver Simsek, Turan
Gunes Bulvari, 41.sokak,
1.Akturk Sitesi No: 8/20, TR-06450 Cankaya, Ankara, Turkey.
E-mail:
[email protected]
Manuscript received: February 22, 2008;
Initial review completed: March 14, 2008;
Revision accepted: April 1, 2008.
|
|
Abstract
We report a case of primary hyperparathyroidism
associated with prolonged hungry syndrome (HBS) after parathyroid
adenomectomy in a 10-year-old girl. Bone mineral density (BMD) revealed
severe loss of cancellous BMD. Overt bone disease, high alkaline
phosphatase, decreased cancellous BMD and a large adenoma can be used as
preoperative predictive risk factors of HBS in children.
Key words: Hungry Bone Syndrome, Hypocalcaemia, Primary
hyperparathyroidism.
|
|
P rimary
hyperparathyroidism (PHPT) is characterized by an increased osteoclastic
bone resorption, leading to osteopenia. Parathyroid resection is the
treatment of choice for patients with declining cortical bone density,
nephrolithiasis, and severe hyper-calcemia(1). One of the common
complications of parathyroid surgery is the development of hypocalcemia.
The incidence of postoperative hypocalcemia varies, due to possible
surgical removal of all parathyroid tissue and long-term hypercalcemic
suppression of nonadenomatous parathyroid glands(1,2). Alternatively,
hypo-calcemia may be due to "hungry bone" syndrome (HBS), which is caused
by massive calcium deposition in the bone after surgical treatment for
PHPT(1). We report prolonged hungry bone syndrome in a 10-year-old child
with a parathyroid adenoma.
Case Report
A previously healthy ten-year-old girl was admitted
with a six-month history of intermittent abdominal pain and easy
fatiguability. A detailed family history ruled out the possibility of
various forms of familial hyperparathyroidism. On physical examination,
there was a genu valgum deformity and a palpable nodule in the
inferior-left lobe of thyroid gland, which was soft and smooth surfaced.
Her height was 145.8 cm (50th percentile), weight 32.7 kg (between 10-25th
percentile), arm-span 139 cm, and blood pressure 110/68 mmHg. Biochemical
investigations are shown in Table I. Elevated serum calcium
levels, decreased serum phosphate concentrations, together with increased
parathyroid hormone (PTH) level confirmed the diagnosis of primary
hyper-parathyroidism (PHPT). Ultrasound demonstrated a large nodule
adjacent to the inferior pole of the left lobe of the thyroid gland.
Technetium-99m Sestaimibi scan gave images which were consistent with a
left-sided parathyroid adenoma (Fig. 1). Roentgenogram of
the long bones of lower extremity revealed demineralization and cystic
lesions (Fig. 2). Bone mineral density (Lunar DPX-L) at the
lumbar spine was 0.5 g/cm 2 and Z
score -2.8. On neck exploration, a well defined mass in the left lobe of
thyroid, 29 x 22 mm in size, weighing 4.2 grams was excised. Light
microscopic examination of the mass revealed a parathyroid adenoma. On the
first postoperative day, the serum calcium level fell suddenly to 7.0
mg/dL. Despite intravenous intermittent calcium supplementation, the serum
calcium further fell to less than 7.0 mg/dL and urinary calcium/creatinine
ratio was consistently less than 0.05. Continuous intravenous calcium
supplementation was given for four weeks and stopped when serum phosphorus
and alkaline phosphatase levels returned to normal limits. Two months
after the operation, she had no symptoms and the BMD at the lumbar spine
increased to 0.6 g/cm2 (Z score -2.05). Eight month after surgery,
the serum prolactin and calcitonin level was measured to rule out MEN 1
and men 2 syndromes and the results were in normal range (6.9 ng/mL and
1.2 pg/mL, respectively).
Table I
Biochemical Characteristics of Patient with Primary Hyperparathyroidism
|
Parathyroid surgery |
Reference |
| |
Before |
after 2 mo |
range |
|
S. total calcium, mg/dL |
12.8 |
8.9 |
8.9-10.1 |
|
S. inorganic phosphate, mg/dL |
2.1 |
4.6 |
3.5-4.7 |
|
S. alkaline phosphatase, IU/L |
1710 |
433 |
130-560 |
|
S. I-PTH, pg/mL (ICMA) |
1027 |
47 |
9-65 |
|
S. calcitriol, pg/mL |
>150 |
54 |
30-65 |
|
Blood urea nitrogen, mg/dL |
12 |
14 |
5-18 |
|
S. 25 [OH] vitamin D, (ng/mL) |
32 |
NM |
34-56 |
|
1,25[OH] vitamin D, (ng/mL) |
>150 |
NM |
30-65 |
|
Spot urine Ca/Cr |
0.36 |
0.08 |
<0.2 |
|
I-PTH, intact parathyroid
hormone; ICMA, immunochemiluminescent assay; NM, not measured;
1,25 [OH]2D3, 1,25-dihydroxycholecalciferol; S. Serum; Ca/Cr,
calcium/creatinine ratio |
 |
|
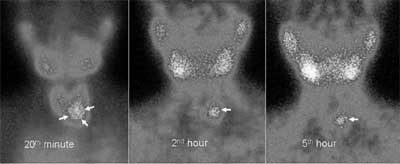
Fig. 1. The images of Technetium-99m
Sestaimibi scan are consistent with a left-sided parathyroid adenoma
(arrows). |
 |
|
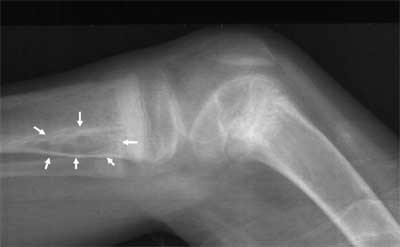
Fig. 2 Cystic lesion (white arrows) and
subperiostal resorption in the proximal metaphysis of the right
tibia, and osteosclerosis in the distal metaphysis of the right
femur. |
Discussion
Hungry bone syndrome is considered to be present if
serum calcium levels are below 8.5 mg/dL and if serum phosphate levels are
normal or below 3 mg/dL on the third day after parathyroidectomy(1). The
predominant feature of the present case is the marked and a longstanding
postoperative HBS. It can be explained by long period of hypercalcemia
secondary to parathyroid adenoma resulted atrophy of the other healthy
parathyroid glands. One previous report demonstrated HBS persisting for 27
weeks post surgery in a case of hyperparathyroidism(3). A long time is
needed by the atrophied parathyroid glands to respond rDA hypocalcaemic
stimulus. Smith, et al.(4) recommended that preoperative
treatment with calcitriol for 5-10 days may prevent HBS in the
postparathyroidectomy state(4). In primary hyper-parathyroidism,
25-hydroxy vitamin D concen-tration tends to be low normal, while
1,25-dihydroxy vitamin D tends to be high normal(5). In the present case,
calcitriol level was extremely high, and there was no indication of
treatment with calcitriol. Bisphosphonates have a negative effect on bone
remodeling and some authors recommended their use to prevent HBS in
patients with PHPT(6,7). Hungry bone syndrome secondary to PHPT is
transient. In this period, calcium supplementation is preferred over
bisphosphonate treatment in children.
Brasier, et al.(1) followed 198 adult patients
after surgery for PHPT and studied the risk factors for development of
HBS(1). They found a positive correlation with ageing, larger adenoma
size, increased serum alkaline phosphatase levels, and elevated blood urea
nitrogen levels. There has been no report on predictive risk factors for
HBS in children with PHPT. Because bone metabolism is more active in
children than adult patients, HBS is more severe and frequent in young
patients with PHPT(5,8). Although most patients with primary
hyperparathyroidism demonstrate preserved verte-bral BMD, which mainly
reflects cancellous bone, our case showed a significant loss of vertebral
bone density. There are a few reports on severe affected lumbar spine bone
densitometry in adults with PHPT, but no report in children with PHPT is
available(9). This finding may indicate that severely affected lumbar
spine BMD at the diagnosis of PHPT may be used as one of the additional
preoperative predictors of HBS in children. The presentation of PHPT in
children is different from PHPT in adults, in whom the disease is usually
less severe(10).
We found a reversible cancellous BMD loss in our child
with PHPT. Overt bone disease, raised alkaline phosphatase, decreased
cancellous BMD and a large parathyroid adenoma may be used as preoperative
predictive risk factors of HBS in pediatric patients with PHPT.
Contributors: ES conceived and designed the study,
interpreted the laboratory tests, and drafted the paper. He will act as
guarantor of the study. YA and YD collected data. MAA is surgeon of the
presented case. ES will act as guarantor for the study.
Funding: None.
Competing interests: None stated.
References
1. Brasier AR, Nussbaum SR. Hungry bone syndrome:
clinical and biochemical predictors of its occurrence after parathyroid
surgery. Am J Med 1988; 84: 654-660.
2. Silverberg SJ, Blezikian JP. The diagnosis and
management of asymptomatic primary hyper-parathyroidism. Nat Clin Pract
Endocrinol Metab 2006; 2: 494-503.
3. Jimenez-Montero JG, Lobo-Hernández E, Picado-Larios
A, Molina MA. Secondary hyperpara-thyroidism after removal of a
parathyroid adenoma. Endocrine Pract 2002; 8: 429-432.
4. Smith D, Murraf BF, McDermott E, O’Shea D, McKenna
MJ, McKenna TJ. Hungry bones without hypocalcaemia following
parathyroidectomy. J Bone Miner Metab 2005; 23: 514-515.
5. Bilezikian JP, Silverberg SJ. Clinical spectrum of
primary hyperparathyroidism. Rev Endocr Metab Disord 2000; 1: 237-245.
6. Khan AA, Bilezikian JP, Kung AW, Ahmed MM, Dubois
SJ, Ho AY, et al. Alendronate in primary hyperparathyroidism: a
double-blind, randomized, placebo-controlled trial. J Clin Endocrinol
Metab 2004; 89: 3319-3225.
7. Kumar A, Raltson SH. Bisphosphonates prevent the
hungry bone syndrome. Nephron 1996; 74: 729.
8. Dempster DW, Cosman F, Parisien M, Shen V, Lindsay
R. Anabolic actions of parathyroid hormone on bone. Endoc Rev 1993; 14:
690-709.
9. Mole PA, Walkinshaw MH, Gunn A, Peterson CR. Bone
mineral content in patients with primary hyperparathyroidism: a comparison
of conservative management with surgical treatment. Br J Surg 1992; 79:
263-265.
10. Kollars J, Zarroug AE, van Heerden J, Lteif A,
Stavlo P, Suarez L, et al. Primary hyperparathyroidism in pediatric
patients. Pediatrics 2005; 115: 974-980. |
|
|
 |
|

