|
|
|
Indian Pediatr 2014;51:
1013-1014 |
 |
Waardenburg Syndrome Presenting With
Constipation Since Birth
|
|
R Gupta, SB Sharma, *P Mathur and
*LD Agrawal
From Departments of Pediatric Surgery, NIMS Medical
College, and *SMS Medical College; Jaipur, Rajasthan, India.
Correspondence to: Dr Rahul Gupta, 202 A, A3 block,
Kamal Apartment- 2,Banipark, Jaipur, Rajasthan, India.
Email:
[email protected]
Received: July 08, 2014;
Initial review: August 04, 2014;
Accepted: September 30, 2014.
|
|
Background: Shah-Waardenburg syndrome is Waardenburg syndrome
associated with Hirschsprung’s disease. Case characteristics: A
10-day-old full-term male neonate of Waardenburg syndrome presented with
constipation since birth along with features of small bowel obstruction.
Observation: Exploratory laparotomy revealed distended proximal
jejunal and ileal loops along with microcolon; an ileostomy was
performed. Outcome: Postoperatively patient developed sepsis and
died. Histopathology confirmed total colonic aganglionosis. Message:
Suspect familial Shah-Waardenburg syndrome in a neonate of Waardenburg
syndrome presenting with constipation since birth or intestinal
obstruction.
Keywords: Shah-Waardenburg syndrome, Colonic
aganglionosis, Hirschsprung disease.
|
|
S
hah-Waardenburg syndrome (SWS) clinically
manifests with pigmentary anomalies, sensorineural deafness and
Hirschsprung disease [1-4]. We report a case of familial SWS presenting
in the neonatal period with features of small bowel obstruction.
Case Report
A 10-day-old full-term male neonate, born to
non-consanguineous parents, presented with bilious vomiting, abdominal
distension and constipation since birth. On examination, the child was
febrile with pulse 180/min, Capillary refilling time >3 sec, respiratory
rate 58/min, and features suggestive of sepsis. He had prominent white
forelock (hair) affecting the anterior, central and lateral part of the
scalp, broad nasal root, and bilateral hypochromic irides. His eyelashes
were also white in color and there was partial albinism. Abdominal
examination revealed distended abdomen with features of small bowel
obstruction.
Hematological and biochemical investigations were
within normal limits. The abdominal roentgenogram revealed dilated small
bowel loops but no air-fluid levels. Barium enema showed a microcolon
with no obvious transitional zone, giving a suspicion of Hirschsprung’s
disease (Fig. 1). Exploratory laparotomy revealed
distended proximal jejunal and ileal loops; microcolon was evident.
Multiple sero-muscular biopsies were taken from unused colon and an
ileostomy was performed. The histopathology confirmed aganglionosis in
the entire colon. A diagnosis of Shah-Waardenburg syndrome was made as
he met all the diagnostic criteria. Post-operatively, the patient
developed sepsis and died.
 |
|
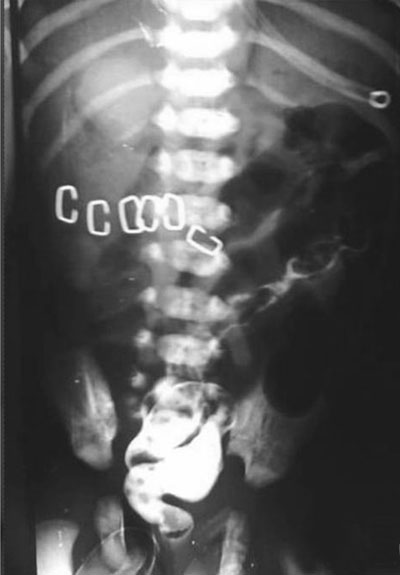
Fig.1 Barium
enema showing microcolon with no obvious transitional zone.
|
On enquiring, one of his elder female siblings had
pigmentary disorder of hair and skin, with involvement of all the hair
on the scalp, eyebrows, eyelashes and heterochromia irides. She was
admitted for intestinal obstruction and died in the neonatal period
three years ago. His father has heterochromia of left eye but not a
white forelock. He also has a broad nasal root and premature graying of
hair. Examination of other family members did not show any features of
SWS or Waardenburg syndrome.
Discussion
Waardenburg syndrome is a group of rare genetic
conditions [1]. Features vary among affected individuals, even among
people in the same family. It has been classified into four types, of
which type IV is also known as Shah-Waardenburg syndrome or Waardenburg
syndrome associated with long-segment Hirschsprung disease [4]. Shah-Waardenburg
syndrome is very rare. Defective migration of the neural crest derived
cell lines, melanocytes and the neuroblasts (contributing the enteric
ganglion cells) during the embryonic phase, has been postulated as a
cause of this disorder [5]. Thus characterizing it as a type of
neurocristopathy [6].
Bowel involvement in Shah-Waardenburg syndrome is
characteristic in the form of aganglionosis in the myenteric (Auerbach)
plexus and the submucous (Meissner) plexus, with long-segment
Hirschsprung disease [7]. The unusual finding in our case was the
extension of the aganglionosis in the entire colon (total colonic
aganglionosis) and familial incidence of Shah-Waardenburg syndrome.
Shah-Waardenburg syndrome have three variants
described on the basis of genetics. Type IVA and type IVB are inherited
as an autosomal recessive trait, while type IVC as an autosomal dominant
trait [8,9]. Folic acid supplementation in pregnancy has been
recommended for women at increased risk of having a child with
Waardenburg syndrome [6].
Patients with Shah-Waardenburg syndrome and total
colonic aganglionosis cases in isolation, usually present within first
month of life with delayed passage of meconium (beyond 48 hours) or
constipation since birth or with features of neonatal small bowel
obstruction (as seen in our case), although cases presenting beyond the
neonatal period have been reported [6,10]. The differential diagnoses of
such presentation are ileal atresia, neonatal small left colon syndrome,
meconium ileus, meconium plug syndrome, and intestinal neuronal
dysplasias. Meticulous attention is required with preoperative
evaluation for co-existence of other system abnormalities, airway
management, and perioperative nutrition strategies.
Initial surgical approach in Shah-Waardenburg
syndrome is histopathological confirmation of diagnosis by routine
seromuscular colonic biopsy and stoma formation depending upon the
involvement of the colon. Frozen section examination if available
remains a useful diagnostic modality for this purpose with its inherent
advantages of prompt intraoperative diagnosis. The definitive treatment
of Hirschsprung’s disease is performed at a later date [10]. Genetic
counseling must be provided for families with this disorder.
Mutational analysis was not possible due to resource
constraints. In conclusion, a high index of suspicion for Shah-Waardenburg
syndrome should be present, in a child, particularly neonate with
Waardenburg syndrome presenting with constipation since birth or with
features suggestive of intestinal obstruction.
Contributors: All authors were involved in all
aspects of case management and manuscript preparation. RG: will be the
guarantor.
Funding: None; Competing interests: None
stated.
References
1. Waardenburg PJ. A new syndrome combining
developmental anomalies of the eyelids, eyebrows and nose root with
pigmentary defects of the iris and head hair and with congenital
deafness. Am J Hum Genet. 1951;3:195-253.
2. Sarin YK, Manchanda V. Shah.Waardenburg syndrome.
Indian Pediatr. 2006;43:452.
3. Farrer LA, Grundfast KM, Amos J, Arnos KS, Asher
JH Jr, Beighton P, et al. Waardenburgh syndrome (WS) Type I is caused by
defects at multiple loci, one of which is near ALPP on Chromosome 2:
First report of the WS Consortium. Am J Hum Genet. 1992;50:902-13.
4. Shah KN, Dalal SJ, Desai MP, Sheth PN, Joshi NC,
Ambani LM. White forelock, pigmentary disorder of irides, and long
segment Hirschsprung disease: possible variant of Waardenburg syndrome.
J Pediatr. 1981;99:432-5.
5. Ambi US, Adarsh ES, Hatti R, Samalad V. Anesthetic
management of Shah-Waardenburg syndrome: Experience of two cases and
review of literature. Saudi J Anaesth. 2012;6:172-4.
6. Sankar R. Shah-Waardenburg syndrome. Dermatol
Online J. 2008;14:19
7. Shim WK, Derieg M, Powell BR, Hsia YE. Near-total
intestinal aganglionosis in the Waardenburg-Shah syndrome. J Pediatr
Surg. 1999;34:1853-5.
8. Egbalian F. Waardenburg-Shah syndrome; A case
report and review of the literature. Iran J Ped. 2008;18:71-4.
9. Syrris P, Carter ND, Patton MA. Novel nonsense
mutation of the endothelin-B receptor gene in a family with
Waardenburg-Hirschsprung disease. Am J Med Genet. 1999;87:69-71.
10. Sharma SB, Gupta R. Total colonic aganglionosis:
A rare entity in children. CIBTech J Surg. 2013;2:58-61.
|
|
|
 |
|

